Summer, 2011
More than 30-million patients in North America receive steroid drug treatment for a broad range of general systemic conditions and skin inflammation. While therapeutic benefits are definitely positive, side effects are common—and of great concern to patients.
Long-term steroid drug treatment has significant side effects, causing damage in several body tissues, including the skin where tissue can atrophy. Impaired tissue repair, or poor wound healing, is one serious complication of steroid drug treatment, or glucocorticoid therapy. Glucocorticoids— a group of steroids naturally occurring in the body and used for anti-inflammatory treatment—affect almost every phase of wound healing due to their inhibitory effects on gene expression in various cells involved in healing. For patients who may encounter accidental or surgical trauma, this effect of glucocorticoids is of paramount concern.
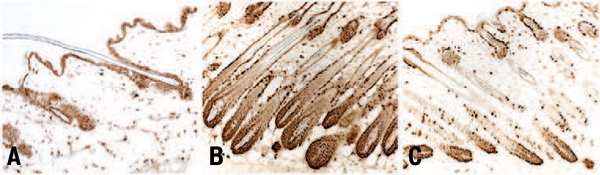
Hair follicles in mouse skin shown in hair cycle stages: resting (A), growing (B) and regressing (C).
Drs. Hannu Larjava and Lari Häkkinen from the Faculty of Dentistry, and Dr. Kelvin McElwee from the Department of Dermatology and Skin Science, UBC Faculty of Medicine, are looking at hair follicle stem cells and the role of an integrin in healing steroid-impaired wounds. Their research, titled “Regulation of Hair Cycle and Wound Healing by αvß6 Integrin,” has attracted five years of funding—just over $564,000—from the Canadian Institutes of Health Research.
Larjava explains the model: “Transforming growth factor beta 1 (TGF-ß1), which is a naturally occurring molecule that regulates skin inflammation and tissue maintenance, strongly inhibits hair follicle stem cell growth and has been directly implicated as a significant factor in hair growth regulation.” TGF-ß1 is produced in the body as an inactive molecule and needs to be activated to function. One of the main activators of TGF-ß1 is an integrin that is expressed on the epithelial cell surface.
“We have recently demonstrated that this integrin is localized in hair follicle stem cells, where it could keep these cells inactive by way of TGF-ß1 activation.” The UBC researchers have also demonstrated that mice engineered to lack this integrin (ß6-/-) have accelerated hair growth and delayed hair regression. Of most consequence, Larjava notes, is that steroid-impaired wounds heal significantly better in ß6-/- mice than in normal mice.
When people receive corticosteroids, these drugs inhibit stem cells, which delays the “re-epithelialization” of wounds. Working under the hypothesis that this integrin naturally suppresses stem cell proliferation in hair follicles, Larjava anticipates that using inhibitors of this integrin could potentially reduce stem cell suppression. This would provide a useful therapeutic tool to improve outcomes of steroid-impaired wound healing.